Everyone talks about skyrocketing drug prices and rising labor costs in healthcare. But what about the hidden culprit quietly draining budgets? Inefficient Healthcare Contract Management. From missed renewals to compliance lapses, poor oversight contributes to nearly 30% of administrative spending—money that could have been redirected to patient care, technology upgrades, or innovation.
The average hospital manages over 1,200 contracts and activates more than 40,000 new pricing line items every six months. In this high-stakes environment, even one missed deadline or overlooked clause can snowball into penalties, delayed reimbursements, or non-compliance with HIPAA and FDA regulations. And while these may appear to be back-office issues, the impact is real: slower vendor onboarding, cash flow disruptions, and resource diversion from frontline care.
This is why healthcare organizations are reevaluating their approach to the healthcare contract lifecycle and the full hospital contract lifecycle. Let’s find out how they’re doing it.
What Is Contract Management in Healthcare?
Hospital contract management isn’t just about filing agreements. It’s about creating a structured, transparent process for handling every contract a hospital, clinic, or health system relies on. These include:
Provider agreements – contracts with physicians, surgeons, or specialists
Payer contracts – insurance reimbursements, Medicaid/Medicare agreements
Vendor contracts – pharmaceutical suppliers, medical equipment providers
Procurement contracts – IT systems, service vendors, and facility operations
Given the scale, organizations need a repeatable, standardized framework that maintains financial accuracy, supports audit readiness, and ensures HIPAA contract compliance.
That’s where the six stages of the contract lifecycle come in, often supported by modern CLM in healthcare tools and workflows.
Exhibit 1: The six stages of CLM (Contract Lifecycle Management) in healthcare.
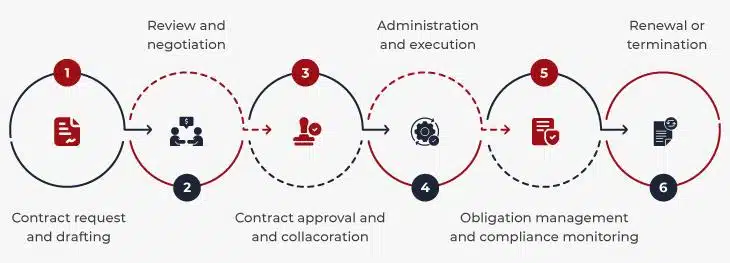
From drafting to renewal, every stage introduces risk if not managed well. For instance, poor negotiation tracking can create unfavorable reimbursement terms, while weak compliance monitoring may trigger costly regulatory penalties. By treating contract management as a lifecycle rather than a one-time administrative task, healthcare organizations gain visibility, accountability, and control.
Key Challenges in Healthcare Contract Management
Every industry struggles with silos and manual approvals. However, contract management challenges in healthcare come with unique layers of complexity. Here are the challenges that make hospital contract management particularly difficult:
1. Regulatory Churn That Ages Contracts Overnight
Unlike static industries, healthcare contracts constantly collide with shifting rules from CMS, HIPAA, FDA, and state-level regulators. A reimbursement clause that was compliant in 2023 may be outdated by 2025. Without active monitoring, hospitals risk billing disputes, denied claims, or penalties tied to stale terms.
2. Clinical Impact of Delayed Agreements
A stalled vendor contract isn’t just a paperwork issue—it can delay the installation of critical equipment or the onboarding of specialized staff. That means slower adoption of new treatments, longer wait times, and in some cases, direct impact on patient outcomes.
3. Multi-Party Complexity Beyond Buyer and Seller
A single healthcare contract often touches hospitals, insurers, GPOs, and regulators. Each party brings its own compliance requirements, performance metrics, and approval hierarchies. This makes alignment harder and increases the risk of version mismatches—another common issue in the broader healthcare contract lifecycle.
4. Data Privacy and Security Overlays
Healthcare contracts aren’t just about pricing—they often include business associate agreements (BAAs) that govern how patient data is handled. With HIPAA violations carrying fines up to $1.5M per year, mishandling privacy clauses is a high-stakes risk. This is why airtight HIPAA contract compliance is non-negotiable.
5. The Usual Pain Points—With Higher Stakes
Healthcare still faces the universal challenges of manual workflows, missed renewals, and inconsistent language. But here, the stakes are higher: a missed renewal might mean losing a payer contract worth millions, not just a delayed vendor invoice.
Solutions to Overcome Challenges in Healthcare Contract Management
Tackling the unique contract management challenges in healthcare requires a blend of technology, discipline, and expert support. Here’s how organizations can address each pain point:
1. Adaptive Compliance Monitoring for Regulatory Churn
As CMS, HIPAA, and FDA rules evolve, contracts must evolve with them. Dynamic clause libraries and regulation-aware CLM tools ensure that reimbursement terms and privacy obligations remain compliant. Quarterly compliance audits paired with automated alerts prevent outdated clauses from slipping through strengthening both operational integrity and HIPAA contract compliance.
2. Fast-Track Approvals to Reduce Clinical Delays
When contracts affect critical equipment or specialized staff onboarding, delays are unacceptable. Automated routing, redlining, and milestone alerts accelerate the approval process. High-priority contracts can be flagged for expedited review, ensuring patient care is never held hostage to paperwork.
3. Centralized Repositories for Multi-Party Complexity
Hospitals, insurers, GPOs, and regulators all need access to the same contract data. A centralized, role-based contract repository ensures alignment and version control. This reduces compliance disputes and allows stakeholders to collaborate securely across the extended healthcare contract lifecycle.
4. Privacy-First CLM for Data Security Overlays
With HIPAA fines reaching $1.5M annually, privacy clauses can’t be an afterthought. AI-driven clause detection highlights missing or risky BAAs, while pre-approved clause templates guarantee consistency. These safeguards hardwire compliance into every agreement before it’s signed.
5. Proactive Governance for the Usual Pain Points
Universal contract challenges, such as missed renewals and inconsistent language, demand proactive governance in healthcare. Contract lifecycle management services offer automated alerts, standardized templates, and integrated dashboards. This shift enables teams to transition from firefighting to strategic oversight, thereby minimizing revenue leakage and compliance risk—key outcomes for optimized healthcare contract management.
Real-World Example: Midwestern Health Network
A Midwestern health system operating across eight hospitals and 120+ outpatient facilities was losing millions due to underpaid claims, delayed reimbursements, and limited visibility into payer contract management. Thousands of contracts were managed manually, creating billing disputes and draining staff resources.
The solution wasn’t technology alone. The network adopted FinThrive’s Contract Manager platform to automate payer agreement management, but they also paired it with a dedicated contract governance team trained to review outputs, flag anomalies, and manage escalations.
This hybrid approach—technology + human oversight—delivered results:
Automation handled routine CLM in healthcare tasks, flagged underpayments, and generated real-time reports.
Specialist teams validated payer performance data, ensured compliance accuracy, and resolved disputes faster.
Administrative burden dropped, allowing in-house legal and finance staff to shift focus toward high-value negotiations instead of chasing paperwork.
The result was predictable cash flow, improved reimbursement accuracy, and faster resolution of disputes—showing that healthcare contract management works best when automation and human expertise go together.
Turning Contracts into Strategic Assets
Contracts are not administrative documents — they are financial instruments, compliance safeguards, and drivers of patient care efficiency.
Healthcare organizations that adopt structured, technology-enabled contract lifecycle management gain:
-
Better reimbursement outcomes
-
Fewer compliance errors
-
Faster vendor onboarding
-
Improved audit readiness
-
Greater financial stability
How Legal Support World (LSW) Helps Healthcare Organizations
Legal Support World empowers health systems with specialized healthcare contract management services, including:
✔ Contract review & summarization
Ensuring accuracy, compliance, and clarity.
✔ Regulatory compliance support
HIPAA, CMS, FDA, and state-level requirements.
✔ End-to-end CLM assistance
Templates, workflows, and document standardization.
✔ Paralegal and administrative support
Frees in-house legal and finance teams to focus on negotiation strategy.
With over 17+ years of experience, LSW helps organizations reduce risk, improve compliance, and achieve operational efficiency across the entire healthcare contract lifecycle.

